When it comes to diabetes, there’s a lot of numbers: number of servings; number of grams of carbohydrate; number of insulin units; number of minutes of exercising; blood glucose number; number of times checking glucose; A1c number; and more. Of these numbers, one of the most common is A1c. For many patients they don’t really understand it but they know if the healthcare provider is happy with it or not. So, what is an A1c . . . really?
A1c’s official name is glycosylated hemoglobin A1c (sometimes called hemoglobin A1c) but, better know as “A1c”. A1c gets its name from:
- Glycosylation: the attaching of a sugar molecule to another substance
- Hemoglobin: the protein substance inside red blood cells that carry oxygen and carbon dioxide in the blood
- Hemoglobin A: type of hemoglobin measured
Glucose in the blood stream glycates or sticks to the hemoglobin for the life of the red blood cell. Normally, red blood cells live approximately two to three months (this is why you get a two to three month average). A glycosylated hemoglobin A1c measures the percentage of red blood cells in the blood stream with glucose stuck to the cell’s hemoglobin A. The higher the blood glucose, the more glucose glycates or sticks to the hemoglobin producing a higher A1c.
While a < 5.7% A1c is considered normal, an A1c less than 7% is associated with good glycemic control for persons diagnosed with diabetes. An A1c
of 8% or more is associated with high glucose levels and increased risk of long-term complications. What A1c is best? The target A1c for a person with diabetes is best individualized in collaboration with their healthcare provider.
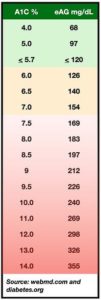
To assist in translating an A1c into day-to-day glucose checks, the A
1c is sometimes interpreted with the “estimated average glucose” or eAG (see table). If you check your glucose with a glucose meter and the meter calculates a multi-day average, this is similar to an estimated average glucose. However, if you only check your glucose pre-meal when glucose levels are usually lower, then the glucose meter average will most certainly be lower than the eAG since the eAG will include post meal glucose levels also. If you check your glucose pre- and post-meal, then the meter calculated glucose level will be a little closer to the eAG value
Since the A1c depends on red blood cells, hemoglobin, and life of the red blood cells, there are clinical conditions that can impact the A1c accuracy: anemia, blood loss, uremia, hemolysis, malaria, pregnancy, smoking, presence of abnormal hemoglobin, and some infections.
There is significant value to an A1c since it provides a snapshot of diabetes management over a two to three month period. It should be remembered though that the A1c is an “average” of glucose values over an extended period of time. If you’ve played with averages, you know that low numbers produce lower averages; higher numbers produce higher averages; and the full story regarding numbers that are high and low can be masked by the final average. This is true for the A1c also.
The A1c cannot capture the following diabetes control information:
- Time in Range (70 – 180 mg/dL);
- Short-term (and potentially problematic) hypoglycemia or hyperglycemia;
- Blood glucose patterns or variance throughout the day
Relying solely on the results of an A1c for management data can hide a blood glucose pattern that includes trends toward low and hypoglycemia at certain times of the day and then be “averaged” out of existence by higher trends and hyperglycemia at other times of the day. Knowledge of glucose patterns are valuable as these patterns can frequently reveal poor control while the A1c supports the opposite.
Persons who are only approved for once a day glucose finger sticks will probably never know if they are having glycemic excursions high or low. Persons checking multiple times a day may never know where their glucose is going overnight. We have technology through continuous glucose monitors (CGM) to answer these questions. Unfortunately, that technology doesn’t have the widespread reach for persons living with diabetes to know their glucose activity around the clock. Indeed many healthcare providers do not fully understand or appreciate the potential value for the CGM technology.
If a person has been living with diabetes for several years, that individual may lose the ability to “feel” glucose highs and lows. That individual believes they are doing a good job managing their diabetes. The healthcare provider commends the patient on their “good work” based on an excellent A1c value. The full situation is not known. While the introduction of a continuous glucose monitor to this patient is not seen as “necessary”, a two-week CGM evaluation has seldom failed to deliver information the patient and the provider did not find valuable.
It is a well established fact that a high A1c is associated with long-term complications such as kidney disease, blindness, heart disease, and nerve damage leading to non-traumatic amputations. What is sometimes lost is we are missing the immediate issues of high and low variations that may impact the person living with diabetes’ day-to-day well-being and safety.
Make no mistake, it is good to have an A1c at least twice a year. Having a clearer image to the background of that A1c via CGM assessment of management every now and then would be helpful also.